Blair Benton is a junior Cardinal Newman Scholar from Benton, Kan. currently studying Pre-Medicine at Newman University. The youngest sibling in her family, Blair chose Newman for its impressive reputation in the sciences and for the numerous scholarship opportunities.

In July 2014, Blair received another opportunity to participate in a medical mission. She was selected to travel to Ecuador, as one of only three medical mission interns, for the International Children’s Heart Foundation (ICHF).
Blair prepared as much as possible but was ultimately blown away by her experience! Read about Blair’s summer spent collaborating with local surgeons, assisting in the operating room and changing lives.
Below is first-hand account by Benton explaining her experience while in Ecuador:
Before traveling to Ecuador, I briefly studied various congenital cardiac defects and Googled clinical presentations and anticipated surgical procedures. As a sophomore in college, I felt this was sufficient preparation for the impending discussions which I would be involved in; however, no amount of internet research or well-intended advice could prepare me for the first patient who walked into the echocardiography lab.
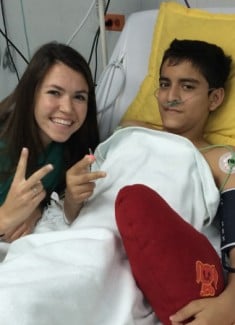
I had come to Ecuador with rose-colored glasses! To me, every kid could be saved, and every outcome was good. I was not prepared for kids to die, but the team surgeon suggested that I select a patient, with whom I identified, and follow that patient through their recovery process. Of course, I chose Joel.
When we began the surgery to repair Joel’s heart defect, the team surgeon and local surgeon worked side-by-side to complete the case, meticulous in every action. The experience of seeing a human heart, and even being able to touch it while it contracted, was extremely humbling.
Joel did exceptionally well during the surgery and continued to improve with each day post-op. Slowly but surely, the snarky teenage antics returned, and Joel “the jokester” kept the entire ICU entertained. On the day that Joel went home, we shared an emotional “goodbye.” It was so incredible to watch him walk out the door, with a world of possibilities within reach: soccer, hanging out with friends, college, and so many other options were no longer hindered by his VSD. Thanks to the operation, he was no longer limited.
Each patient had their own personality, story and unique obstacles to overcome, but the one thing they all shared was the impact they had on my life. I’m usually terrible with “goodbyes,” but each child leaving our ward signified a difference being made and the chance for a better future.
Throughout the mission, I experienced many “firsts.” I saw the general anesthesia process for the first time, witnessed the placing of intravenous and intra-arterial catheters and even had the honor of scrubbing for an open heart surgery! Most importantly, it was the first time I was able to comprehend the intensity of the trust each patient has in his or her physician. Each child had unconditional faith that we could take care of them.
Joel was just one of 19 patients on whom we operated during our two week stay in Guayaquil, Ecuador. Seeing new patients could be frustrating, especially when we found a child beyond our capabilities, but at the same time, those patients reaffirmed the reason for ICHF missions. We were there not only to operate on these children, but also to educate the community about early recognition and treatment of the congenital defects. This was the epitome of the mission—two different worlds coming together, learning, and teaching, all with the goal to help children.

