Scrubs, a hospital gown, gloves, an N95 mask topped with a standard mask, eye goggles, a face shield, a hair cap topped with another cap — this is Salma Rios’ uniform. She wears it for 12-hour shifts several nights a week.
Rios is a 2020 Newman University nursing program graduate. She worked as a certified nursing assistant for one year at Ascension Via Christi St. Francis while completing her Bachelor of Science in Nursing.
After passing the National Council Licensure Examination in June, Rios stepped into a full-time night shift nurse role in the COVID-19 intensive care unit (ICU) at St. Francis.
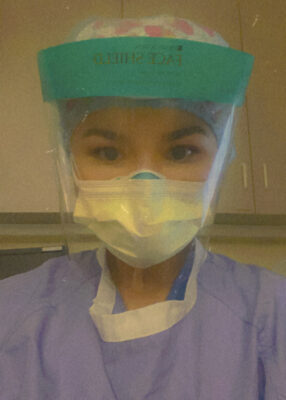
Starting a nursing career in the middle of a worldwide pandemic wasn’t as smooth of an adjustment into her career as she’d hoped. She knew immediately that there was no way to go about it other than to just jump in and work.
“Being a new grad with a new pandemic, it’s just a big slap of reality,” exclaimed Rios. “These patients are super sick. In the medical ICU, as a tech, I saw some sick patients but nothing compared to what it’s like having one COVID patient. There is just so much going on with them.”
Her first week as a nurse was also the first week the hospital converted its medical ICU into its COVID ICU.
Roz Hutchinson, Ascension Via Christi director of communications and public relations, said the ICU transition was necessary due to growing rates of COVID hospitilizations.
“You don’t want to mix patients when you’re dealing with an infectious disease. There are a whole different set of protocols when you’re dealing with a pandemic. This week (Oct. 16), as a community, we hit the highest number of COVID patients to date. We had nearly 50 at St. Francis and more than 20 are in the COVID ICU.”
Hutchinson said Rios is doing an amazing job helping patients, referring to her as a “rock star” in the unit.
“She was in the ICU last year, but this year, the average number of deaths in that unit is much higher and the frequency that she’s dealing with end-of-life issues has greatly increased.”
Hutchinson said when nurses enter that unit, there’s no getting a drink or going to the bathroom, until you leave that unit for a break. Typically, that’s about every four or five hours and during that time, they are dressed in full PPE (personal protection equipment).
“That’s a lot to deal with, both physically and emotionally. And to see Rios, a brand new nurse who handles it with such poise and assurance, it says a lot about her as a person and a lot about her training.”
Rios said she just takes one day at a time, following the guidelines and suggestions they receive from the Centers for Disease Control and Prevention, the Sedgwick County Health Department and the hundreds of doctors and nurses in and beyond the state of Kansas who share newly learned information.
Because COVID-19 is such a new phenomenon, they are learning something new about treatment and care every week, even daily.
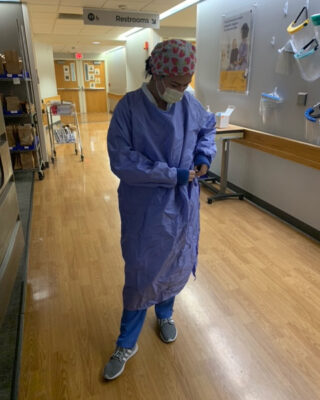
The work environment and the staff she works with act as a system of support.
“We are fatigued and exhausted, physically, mentally and emotionally,” said Rios. “Even seasoned nurses are struggling. But the positivity is high, we are helping each other out, giving each other breaks as often as we can.”
That positivity is what keeps her going. As COVID cases come and go in waves, she and her colleagues rely on their training and experience to work on the front lines and do what they can to save as many lives as possible.
Rios said her education at Newman was very helpful, especially in the first months as a certified nurse.
“It really goes back to the fundamentals, and that first year of the program. Those basic things — talking to families and patients, being sterile, practicing skills — much of what we learned in year one is what I’ve applied.”
She added that the only thing she didn’t feel fully prepared for was the type of patient interaction that comes with a pandemic. Because of the overhaul of visitation policies in hospitals nationwide, family interaction has become more difficult and emotional.
“Families are calling or using FaceTime now. Not being able to communicate in person has been heartbreaking. In a pandemic situation, it’s just scarier for the patient and their families, and through all that, during the bad times, we have to be realistic with the family members; about end-of-life and the reality of what’s happening to their loved one.”
She envisions nursing programs everywhere will add additional communication skills training into their curriculum. Health care professionals are seeing alarming death rates due to an infectious disease they’ve never had to deal with before and they are finding there is somewhat of a learning curve.
“It’s a good day at work when someone doesn’t pass away,” she said. “That’s the environment right now. Sometimes we are hurting with them. Being able to communicate, being straightforward and giving them a real image, you have to find that balance.”
At the end of the day, Rios said keeping a positive attitude is the best everyone can do.
Her co-workers and supervisor act as a sounding board when needed, and they often debrief at the end of each shift, talking with one another to release some of the stress and heaviness they feel on a daily basis.
“Just keeping that positive attitude and being positive about everything at work and everything overall in life,” she said. “You just have to be positive at the end of the day and do what you think is best. If you’re not positive at work, if you come in with a black cloud, that doesn’t do anyone any good.”

